Sierra Leone
Three and a half hours from Freetown, in the district of Bombali, a car rolls along a dirt road and stops at a remote village. The entrance to the village is cordoned off with yellow police tape. Two soldiers in camouflage stand in front. Beyond the village lies dense rainforest.
The car doors open, and two women get out. One is Wafaa El-Sadr ’91PH, University Professor at Columbia and the director of two centers at the Mailman School of Public Health: ICAP, which works internationally to fight major health threats, and CIDER, the Center for Infectious Disease Epidemiologic Research.
What startles El-Sadr immediately is the silence. She has entered many African villages in her career, and always they are full of life: kids playing, people moving from house to house. But in this village, which has lost dozens of people to the Ebola virus, everyone is indoors. The village — a thousand people, most of them children — is under quarantine. El-Sadr has a word for how it feels: unnatural.
The other woman is Susan Strasser, the director of nursing for ICAP. Strasser has lived in Africa for most of her adult life. A Rochester native, she spent the past eight years in Zambia, where she was the director of an AIDS foundation, before coming to Columbia last July. It is late October now.
As a nurse, Strasser has been in some tough spots. She lived in South Africa during apartheid, and worked at a rural hospital in Zimbabwe, delivering babies at a time of rising HIV infections. But what’s happening in West Africa is unlike anything she has seen.
From the moment they boarded the plane bound for Sierra Leone, Strasser and El-Sadr had found themselves in a world completely dominated by Ebola. The flight attendants wore gloves and masks. There were vats of chlorinated water at the airport and at the hotel in Freetown. Everywhere they went, health officials took their temperature. Billboards reinforced the “no touch” mantra. It was strange, and very difficult, not to hug or shake hands. When you met people, you had to check your normal impulses and hold your hands together.
All the schools were closed, including medical schools and nursing schools. Though life continued in the city, there was a notable absence. Usually in developing countries during a humanitarian crisis you saw all the NGOs whizzing around in their logo-marked trucks. Not here. Fear and lack of expertise have kept agencies out. You know you’re watching history, Strasser would later say. You know you’re watching something very bad play out.
In Freetown, a port city of 1.2 million, El-Sadr and Strasser had met with local and international agencies to see what ICAP could do to help stop the epidemic. One meeting was with Sierra Leone’s chief nursing officer. In Strasser’s experience, Africans were very modest about their struggles, and so it was striking when the woman looked at her and said, “It’s been really hard.” That was telling. Hundreds of health workers had died of Ebola in West Africa. There were few doctors and nurses to begin with — years of war had seen to that — and now to care for patients was to risk your life.
El-Sadr and Strasser are accompanied to the quarantined village by John Redd ’94PH, an epidemiologist from the Centers for Disease Control and Prevention (CDC). Redd has been to this village many times.
The Americans show their IDs to the soldiers, who take their temperatures with a forehead thermometer — all normal — and admit them past the yellow tape. On the other side, the village chief, from ten feet away, greets them. Strasser asks him if the village has received food. Quarantined villages are supposed to get food from the UN World Food Programme, but the food doesn’t always make it. To enter a hunger-stricken village could cause unrest. The chief affirms that the food arrived.
El-Sadr and Strasser then meet, at a distance, with the pastor. The pastor’s wife died from Ebola. So did all his children.
So did all his grandchildren. He is a broken man. It was horrible, Strasser will later recall, absolutely horrible. In the houses, people sit, just waiting, waiting. Waiting for the twenty-one days to pass, the limit for the virus’s incubation period.
There are other visitors in the village: two community-health workers serving as contact tracers. Contact tracing is one of the oldest ways to fight outbreaks of direct-contact diseases. The contact tracer’s job is to get the names of those who have had contact with a patient, find them, and monitor them for symptoms. The sooner you isolate a sick person, the more new cases you prevent.
Now a woman in a house tells one of the contact tracers that she is ill. This is not an easy thing to admit, given the awful fears: separation from one’s family, pariah status, unthinkable pain and suffering, a solitary death, an unsanctified burial. Still, the early symptoms of Ebola — fever, headache, fatigue, sore throat — are similar to other, less extreme diseases.
It’s malaria, she says. It’s just malaria.
A common enough malady, but you can’t distinguish it without a blood test. The woman’s husband, who was sick with Ebola but has since recovered, is with her at the house. The woman refuses to go to the nearby holding center, where sick people can be isolated, tested for Ebola, and given Tylenol and oral-rehydration salts. Holding centers have a reputation as grim, death-filled places.
The contact tracer speaks with Redd, who then addresses the woman, again from an abnormal distance. He tells her that it’s in her best interest, and in the community’s best interest, for her to go to the holding center. Finally she agrees to go.
Then the other contact tracer says that he, too, is feeling sick. I want to go to the holding center as well.
Many of the complications of the epidemic are on view this day, in this village. El-Sadr and Strasser, standing in the tropical heat, take note of all they see.
"Don't bury the dead. Don't touch the sick."
Broadcasting from high atop Leicester Peak, above the green hills and corrugated tin rooftops of Freetown as it rambles down to the sea, it’s Star Radio 103.5, live on the air. “Wash your hands. Simple hygienic techniques will get rid of Ebola. People are still washing bodies and inviting people into quarantined homes. If this continues, the Ebola still stay.” On this Sunday in November, as cases in Sierra Leone soar past six thousand, with 1,500 deaths, some Sierra Leonean journalists are in the studio, discussing the epidemic. “We can stop Ebola only if we change our attitudes,” one man says. Another laments how Sierra Leone is portrayed by outsiders. “The international media look for the negativity when it comes to Africa — war, poverty, pestilence. Not everyone is dying in Sierra Leone. People fear the virus because of what they hear in the media. You and I sitting here have nothing to fear from the virus.” Rather, he says, it’s in the remote villages and the slums that “Ebola caught us pants down.”
The same weekend, another voice is heard on Star Radio. Adeyinka “Yinka” Akinsulure-Smith ’97TC, a psychologist and associate professor at City College of New York, joins a conversation via Skype. Akinsulure-Smith was born in Sierra Leone and speaks Krio, an English-based creole that is the lingua franca of the former British colony. Her parents taught at a university in the south, and she grew up 120 miles from Freetown. After high school, she lived in England, Canada, and the US. She has been going back to Sierra Leone ever since.
HOST: Dr. Yinka, people go through things. Some people cry. They cry a lot. What would you say to such people?
DR. YINKA: I would say, “You are not alone; others are going through it, too. Yes, cry a little, but understand that you are not alone. Others have similar problems. Reach out, call people on the phone. Don’t isolate yourself.”
Akinsulure-Smith has long been a voice for Sierra Leoneans. When asylum seekers from Sierra Leone’s civil war (1991-2002) began arriving in New York, she cofounded an organization called Nah We Yone, which in Krio means “It Belongs to Us.” The group helped people, some of whom had been maimed by diamond-funded rebels, find psychosocial and legal services and apply for asylum. Soon, Nah We Yone, assisted by students at Columbia’s School of Social Work, extended its outreach to the Sierra Leonean diaspora.
The war destroyed much of Sierra Leone’s infrastructure and killed seventy thousand people in a country of less than five million. Still, as time passed, things began to improve. Schools reopened, expatriates returned. People were regaining their foot-hold. Then, last spring, Ebola came.
The new crisis, piled atop the old one, spelled catastrophe. Many people didn’t believe the virus existed. Others attributed it to bad witchcraft or foreign plots. The virus spread, and so did fear. Bodies were being dumped because people didn’t want others to know that someone in their family had Ebola.
“During the war, we knew where to go and whom to avoid,” says Akinsulure-Smith. “Ebola creates a whole other element of avoiding people. Families have been divided. Children are sick and dying, but you can’t touch them. I’m a mother. I have two kids. I cannot fathom seeing my kids in distress and not being able to hug, stroke, caress, or comfort them.”
Thousands of children have lost one or both parents, causing further social shocks. Children are traumatized by loss, separation, the suffering of family members, the terror of strangers in hazmat suits taking loved ones away, the lack of support services, and a pernicious social stigma.
Akinsulure-Smith is involved with a group of psychologists and psychiatrists in the US and Europe called the Sierra Leone Mental Health Initiative, which studies the country’s postwar mental-health needs. When Ebola struck, the group wondered how it could help from afar — how could it reach the wider population, give people a place to talk about their experiences, their emotions?
Because Sierra Leone has low literacy rates and scant Internet access, most people get their information by radio. And so the group decided to produce a radio show: four hour-long segments on the independent Star Radio. Akinsulure-Smith could call in, and people throughout the country could listen.
DR. YINKA: We’ve been talking about adults, but children also can have these mental-health challenges, these stressors. We have to remember that their reactions, the way they feel, the way they behave, can be different from adults. So we have to adjust for them, too. Crying, nightmares, regressive behaviors — it’s not that they are choosing to behave badly. You can’t just beat them.
Recently, the Christian development organization CBM trained twenty-one psychiatric nurses to help the public cope with the myriad mental-health problems caused by the epidemic. Now, Akinsulure-Smith is looking into another use for telecommunication: the long-distance supervision of these nurses.
“Unfortunately,” she says, “one of the nurses just died of Ebola.”
Guinea
The outbreak began in December 2013 in a village in Gueckedou, in southern Guinea, near the border of Liberia and Sierra Leone. Months later, investigators traced the source of the epidemic to a two-year-old boy named Emile. It appeared that Emile had contact with a fruit bat, the animal widely thought to be the virus’s natural host. After four days of fever, vomiting, and bloody diarrhea, Emile died. Then his sister got sick and died, then his mother, then his grandmother. The bodily secretions of Ebola victims are most infectious at the time of death, and anyone handling a body for burial is at risk of catching the virus. This is what seems to have happened in Gueckedou.
By April, eighty people had died in Guinea, and the virus had gotten into the capital, Conakry, a city of 1.7 million — a grave event, as previous Ebola outbreaks had been confined to sparsely populated areas. Picture, then, the branching patterns of transmission, the points and lines multiplying and crisscrossing, going from village to town to city to village, in a widening meshwork of out-of-control contagion. Flung into this web is the contact tracer, who must follow the lines, untangle them, and cut them off. The obstacles are dizzying: huge geographic expanses, bad roads, poor infrastructure, meager resources, and, among the populace, a fierce distrust of foreigners.
Anne Liu came to Guinea with a plan. Liu is the lead manager of the community-health worker program of the Millennium Villages Project at Columbia’s Earth Institute, where she sets up health systems for maternal and child health. Now she and her team (five from Columbia, two in Guinea) are building a system to help stop an epidemic of global range, using a technology that is commonplace in much of the world: smartphones. “Our goal is to prevent further transmission by being able to track the entire chain of response once you identify an Ebola case,” Liu says. “We’d be able to see if there were any gaps.”
The chain of response is this: contact identification, contact tracing, diagnosis (lab results), treatment (outcomes at the tent-based Ebola treatment units, or ETUs), burials (safe or unsafe?), and community awareness. The phones would allow all the partners — contact tracers, doctors, lab technicians, NGOs, and the government — to share data instantly in a region where it can take days just to transport a blood sample to the nearest lab. If the enemy is time, the weapon is speed.
“To catch up with and beat Ebola, we need to substantially scale up our response,” the Guinean president Alpha M. Conde announced on September 18. Conde had been having discussions with Jeffrey Sachs, the Earth Institute’s director. “The immediate deployment of community-health workers,” Conde stated, “trained and equipped through an initiative of professor Jeffrey Sachs from Columbia University, will accelerate and strengthen our national response to Ebola, as well as structure a response at the level of our local communities.”
A month later, Liu is in Conakry, meeting with UN agencies and NGOs in the lobbies of the two hotels where everyone is working and, disappointingly at such a critical hour, squabbling. Liu’s objective is cohesion: to turn a slow paper-based system into a nimble digital one, in which everyone in the response chain can send, receive, and access information in real time. The plan calls for two thousand smartphones for two thousand contact tracers, and another five hundred smartphones for workers in labs, treatment centers, and government and nongovernment agencies.
Ericsson has donated a thousand phones. The phones use the mobile medical-software program CommCare, created by the company Dimagi, which is working with the Earth Institute on customizations for the contact-tracing protocols of this epidemic. Users will need Edge, 3G, or Wi-Fi to submit data. If they’re out of network, the program saves the data, then sends it when they reach a network. Meanwhile, the UN Emergency Telecommunications Cluster (a group of organizations that works to coordinate communications during humanitarian crises) and companies like Facebook are looking to expand Internet connectivity in Guinea’s forested region.
In early November, Liu, after a short trip to New York, is on her way back to Guinea to train the people who will train the contact tracers in the mobile-phone system. At this point, two thousand Ebola cases have been reported in Guinea, with more than 1,100 deaths.
Liberia
“Whoa, they just found Ebola in Guinea,” said Ashoka Mukpo’s girlfriend last March. She was reading an article in Mukpo’s apartment in Monrovia, Liberia.
Mukpo ’12SIPA got a little nervous. Guinea and Liberia shared a 350-mile border. Well, that’s scary, he thought, but that’s not going to affect us.
Mukpo had first come to Liberia in 2011. Columbia’s Center for International Conflict Resolution had hired him to do a research project in Liberia through SIPA’s professional-development program. His job was to work with the UN peacekeeping mission to evaluate how the rush of foreign investment after the country’s 1999-2003 civil war was affecting the peace-building process. Liberia had a long history of turmoil over its natural resources, and there was concern at the mission about how the investment projects were sitting with local communities. Mukpo co-authored a report on investment and community relations, based on field interviews and talks with Liberian officials. In Mukpo’s view, many contracts were being imposed from the top down. Dissenting voices were ignored. Projects ought to be monitored, he felt, to make sure they didn’t stir up regional factionalism, antagonize communities, or bolster perceptions that the government was corrupt and negligent of the poor. There were a few NGOs that did that sort of work. Mukpo approached one group, called the Sustainable Development Institute, and offered his services as a writer and researcher. The group hired him, and Mukpo moved to Liberia full-time.
Now, in March 2014, the word “Ebola” was popping up.
“First we heard that it was under control, and then there were rumors that someone with Ebola traveled to the Firestone hospital from the Guinea border, which is quite a distance,” says Mukpo, thirty-three. “When we heard that, we tensed a little and thought, ‘If someone with Ebola made it all the way to this hospital, even past Monrovia, that could be a problem.’ Then things quieted down. For about a month, we didn’t really hear about any new cases. A few cases had been treated, but the government was very clear: ‘Ebola’s here, you need to watch out for it, you need to observe some safety protocols, but we have it under control.’”
Mukpo’s contract ended in May. When he went back to the US that month, the mood in Liberia was not one of panic. “The expats were afraid,” Mukpo says, “but the Liberians thought the whole thing was a lie. Not all Liberians — obviously there were Liberians who understood that this was a real medical crisis — but most people didn’t worry about it because they felt like it was a hoax, a scam by the government to get foreign aid. This is where history and the present intersect. There’s this historical dynamic of the central government exploiting the rural people — the settlers from America and their descendants ran the country, and there wasn’t much opportunity for indigenous people from rural areas, which was one of the main causes of the war. Now you have a government that’s been supported by donor organizations, NGOs, and the UN, and which has promised a more egalitarian system of governance. But my experience in Liberia was that the corruption and accountability issues have not been effectively addressed.”
In July, Ebola resurged. Mukpo, who was home in Providence, Rhode Island, saw reports that more cases were being found in Liberia — and then it was in Monrovia.
“I watched it on a week-by-week basis go from concerning to very alarming,” Mukpo says, “to a point that I started worrying about what it was going to do to the social and political fabric of the country.” He wrote articles examining the sociopolitical effects of the crisis and why things were spiraling. “I think if people had had more of a sense that their government was honest and had their best interests in mind,” he says, “they probably would have adopted preventative measures much quicker.” Mukpo saw a lot of discontent with the government of Ellen Johnson Sirleaf, Africa’s first female head of state and a Nobel laureate who was first elected in 2005. “If you look at the 2011 elections, the first round, she didn’t even win the majority of the votes. This is already a government that’s not terribly popular, and suddenly there’s this medical crisis that many are blaming on the government.”
Mukpo’s worst fears started to be realized in August, when he read about what happened in the Monrovia neighborhood of West Point. The balcony of Mukpo’s Monrovia apartment overlooked West Point, and Mukpo knew some of the seventy thousand people who lived in that maze of tin-roofed shanties. He knew their level of political mistrust. When some residents looted an Ebola treatment unit, resulting in the escape of seventeen patients and the theft of bloody bed sheets and medical equipment, the army placed the entire neighborhood under quarantine. Mukpo watched from afar as troops opened fire on Liberians “who didn’t understand why they’d even been quarantined in the first place,” he says. “They still felt that the threat wasn’t real.”
Mukpo had a media-studies background, and with a disaster unfolding in a country he loved, he considered returning to Liberia to report on it. “Professionally and personally, it was difficult for me not to want to go back when there was this massive crisis,” he says. “I just made that decision and said, ‘I’m going back.’”
His family tried to dissuade him, but Mukpo felt he had no choice. He landed in Monrovia in early September, to a situation that he was unprepared to see firsthand.
New York
“I want us to be on the ground tomorrow,” says Wafaa El-Sadr, seated in her office at the Mailman School of Public Health on West 168th Street. “I’m convinced we can actually make a difference. That makes it very hard to sit here.”
It is mid-November. El-Sadr and Strasser have been back from Sierra Leone for two weeks. Like anyone coming to the US from West Africa, they are required by the CDC to take their temperature twice daily and answer questions from the health department. Since neither of them worked inside an ETU, there is virtually no chance of their having caught the virus. In Sierra Leone, meanwhile, Ebola is spreading.
One big problem of the epidemic has been a lack of holding centers. In response, the British government, through the UK Department for International Development (DFID), is funding the building of “community care centers” — multi-bed units located near villages and staffed by laypersons rapidly trained by the British army. The idea is that patients will be more inclined to self-isolate if they know they’ll be closer to their families while awaiting their lab results. People who test positive for Ebola would be transferred to an ETU, like those run by Medecins Sans Frontieres (Doctors Without Borders). There is talk about ICAP evaluating these centers for safety and efficacy once they are functioning.
El-Sadr and Strasser, based on what they saw in Sierra Leone and on their experience fighting HIV/AIDS, have also drawn up a proposal to the CDC for a long-term strategy to improve the tracking of cases, expedite the turnaround of lab results, and — most ambitiously — find and train nurses.
“The number of health-care workers who have died in this outbreak is substantial, and particularly nurses,” El-Sadr says. “Nurses are very precious — they provide the care.” Many on the frontlines have died, and those who haven’t died have watched their colleagues die. Even before Ebola, there were about two nurses for every ten thousand people in Sierra Leone.
Yet ICAP found that the prevailing assumption — that there were too few nurses to staff the new care centers — was incorrect. Organizations working in Sierra Leone could identify nurses who were ready and willing to respond, including unemployed and retired nurses.
“As we rush to find trained health workers, it is essential that we keep them safe,” Strasser says. “Buddy systems and on-site supervision are helping, but we need more. We’ve seen a situation spin out of control due to poor health systems. Nurses are at the forefront of these systems, and they’re the ones most at risk.”
On February 26, 1969, John Frame ’66PH, a doctor in the Division of Tropical Medicine at Columbia’s school of public health and the medical director of a network of Christian hospitals in East Africa, received a call from Nigeria. The caller was Jeanette Troup, a doctor at the missionary hospital in the town of Jos. Troup told Frame that a mysterious illness had broken out at the hospital. Two American nurses, Laura Wine and Charlotte Shaw, had developed fevers that progressed to nausea, hemorrhaging, organ failure, and death. Antibiotics were ineffective. Troup had performed an autopsy on Shaw, with help from the hospital’s head nurse, Penny Pinneo. The autopsy revealed multi-organ devastation.
Now, a week later, Troup said, Pinneo had a fever and mouth ulcers.
Frame ordered Pinneo flown to New York immediately. The fifty-two-year-old nurse was evacuated from Nigeria, along with blood specimens from her fallen colleagues. While Pinneo was being transported, Frame contacted virologist Jordi Casals at Yale, and told him to expect some blood samples.
At JFK Airport, Frame met the ailing Pinneo and drew her blood. An ambulance took Pinneo to Columbia-Presbyterian Hospital. There, she was placed in isolation. Frame sent all the blood samples to the Yale lab, where Casals and his colleagues set to work to identify the pathogen. Pinneo was acutely ill. At one point, her temperature reached 107 degrees. Somehow, she survived. By early May, after nine weeks in the hospital, she was released.
A month later, Casals, who lived on Manhattan’s Upper West Side, began to feel sick. He thought his symptoms were unrelated to the mystery bug at his lab. But his doctor, Edgar Leifer ’42GSAS, ’46PS, a professor at Columbia’s College of Physicians and Surgeons, convinced him to go to Columbia-Presbyterian. Like Pinneo, Casals was placed in isolation under Frame’s care. As Casals’s condition worsened, and increasingly resembled the unknown disease he was studying, Frame called Pinneo, who lived upstate, and asked her to fly to New York to donate her blood, which had antibodies. Pinneo did. Casals received injections of Pinneo’s serum and recovered.
But in November 1969, Juan Roman, a technician at the Yale lab who hadn’t been working on the virus, fell ill with the same symptoms. His sickness, which ended in death, caused great alarm: no one knew how he’d contracted the disease, and even Casals, meticulous in his own laboratory caution, couldn’t be sure how he himself had gotten it. The lab was shut down.
That winter, at the mission hospital in Nigeria, Jeanette Troup saw more patients with symptoms like those of nurses Wine, Shaw, and Pinneo. To verify her hunch that it was the same disease, Troup did an autopsy on one victim. In the process, she cut her finger. Days later, she was sick. In New York, Frame, having heard about Troup’s illness, asked Pinneo and Casals to fly to Nigeria to donate their antiserum. They agreed to go. Pinneo arrived on February 20, 1970, only to learn that Troup had died two days earlier.
By then, the new virus, whose natural host was the multimammate rat, had been isolated. Frame named it Lassa fever, after the Nigerian town where it first appeared.
It wasn’t until 1976, in Central Africa, that another, more deadly hemorrhagic virus emerged.
William T. Close ’51PS was living in Zaire at the time. Close had lived there since 1960, when he and his wife came with an American missionary group. The country was called the Belgian Congo then. Just after Close’s arrival, Belgium granted independence to its resource-rich colony, and the Republic of the Congo was born. Violence promptly erupted, both against the Belgians and between Congolese political factions. The 1,500-bed hospital in the capital, Leopoldville, had one surgeon. Close heard about this shortage and went there to help. The injured poured in, and Close sewed up a lot of people.
One day, Close was summoned to the home of the army chief of staff, Joseph-Desire Mobutu. Colonel Mobutu wanted Close to remove a fishbone from his great-aunt’s gullet. Close obliged. Soon after, the country’s first prime minister, Patrice Lumumba, a strident anti-imperialist, was toppled in a coup led by Mobutu and backed by the US and Belgium, and later executed. Close was made chief physician of the army. He also became Mobutu’s personal doctor.
In 1971, Mobutu, as president, pursued a program of Africanization. He changed the country’s name to Zaire, the capital’s name to Kinshasa, and his own name to Mobutu Sese Seko. By then, Close was growing disillusioned with Mobutu. To his eyes, the president had gone from a charming, compassionate leader to a detached, wealth-amassing tyrant. In the summer of 1976, Close went on leave to Wyoming, where he planned to set up a rural practice. In October, he got a call from the Zairean health minister, who told him of a strange disease that appeared in August in the northern village of Yambuku, six hundred miles from Kinshasa. Victims died quickly and horribly, with external hemorrhaging. Panic had gripped the capital, and the military was avoiding the hot zone up north. Mobutu was rumored to have fled to France with his family.
Close flew back to Zaire. On the flight from Geneva to Kinshasa, he sat near Joel Breman and Karl Johnson, two epidemiologists sent by the CDC to investigate the disease, which had infected some three hundred people, killing 90 percent of them. The investigators faced towering questions. How was the illness transmitted? How had it spread? How could it be stopped?
Close overheard the discussion and introduced himself. The three men talked through the night. When they landed in Zaire, the charismatic, French-fluent Close began forging order from chaos: as the director of the country’s biggest hospital, he secured medical equipment and supplies; and as the president’s doctor, he convinced a wary Zairean air force to provide a C-130 cargo plane to take a Land Rover and materiel up to the jungle-bound village of Yambuku. He obtained helicopters, too, so that the investigators could visit the hundreds of neighboring villages in their quest to halt the disease. One of Close’s children, the actress Glenn Close, wrote of her father, who died in 2009, “His was the kind of vitality that immediately changed the chemistry of whatever space he entered — a true life force.”
The response team reached Yambuku. There, the investigators found that a high rate of infections occurred in young women. Hospital records showed that many of the women had been pregnant. It turned out that the Flemish nuns who ran the local clinic had given the women vitamin injections with reused, unsterilized needles. The case was cracked: Ebola, named for a river near Yambuku, was spread through bodily fluids. Now, under Close’s logistical command, the team made its way to villages to find and quarantine the sick, using the medical equipment and protective gear that Close had marshaled. Years later, Peter Piot, the Belgian microbiologist who isolated the virus and who was part of the team in Zaire, referred to Close’s role in stopping the world’s first recorded Ebola outbreak as “indispensable.”
By December 2014, reported cases in the current outbreak approached twenty thousand, with around seven thousand deaths. The death toll of all twenty-four previous Ebola outbreaks combined was 1,590, according to the World Health Organization (WHO). Unlike those outbreaks, this one crossed borders and got into big cities like Monrovia, Freetown, and Conakry — the capitals of nations still recovering from wars, where public-health infrastructures are almost nonexistent, and where doctor-patient ratios are woefully low. Liberia, for example, a country of 4.3 million, has about fifty doctors.
In some ways, the health infrastructure in parts of Africa hasn’t changed much since the 1960s, when Bill Close was one of three doctors at the main hospital in Kinshasa, performing cranial surgery with a carpenter’s drill.
Liberia
Ashoka Mukpo left Providence and flew back to Liberia in September. On his first day in Monrovia, he saw bodies lying in front of a treatment center. One of them was a child.
He listened to parents talk about how they’d spent days driving around in vain to find a facility that would take their son. They were forced to watch the boy die in the car.
People couldn’t get treatment. There weren’t enough ambulances. Bodies were decaying in homes. “The depth of human suffering was much more than anything I’d ever seen,” Mukpo says. “Life in Liberia was already very difficult, and nobody needed this.”
In Monrovia, he encountered a city steeped in anxiety. While you could still go to the beach and have a great afternoon and not even discuss Ebola, just tell jokes and drink beer, the underlying energy was concern for the future and an awareness that nobody knew how bad things were going to get.
Mukpo had come this time as a journalist. A friend was working on a documentary about Liberia, and had offered to pay Mukpo’s way if he would help her shoot. Mukpo, who had some experience with a video camera, agreed.
The case count swelled. Each day, dozens of sick people were turned away from treatment centers. They could either go to a government holding center and wait in a cot or on the floor with other patients, or they could go home, where they risked infecting family members and neighbors.
On Tuesday, September 30, Mukpo was hired by NBC News to be the second cameraman for Dr. Nancy Snyderman, the network’s chief medical correspondent. The next day, he began to feel tired and achy. He took his temperature and saw that he was running a fever of 101.3. Frightened, he quarantined himself, and on Thursday morning he visited a Doctors Without Borders treatment center to get tested. The results came back that night. Mukpo had Ebola.
By Sunday he was on a plane back to the US, to the biocontainment unit at Nebraska Medical Center in Omaha. Like CUMC assistant professor Craig Spencer ’13PH, a Doctors Without Borders volunteer who contracted Ebola in Guinea and was treated at New York’s Bellevue Hospital, Mukpo benefited from excellent care. His treatment included serum from an Ebola survivor, the missionary doctor Kent Brantly, who happened to be driving through the Midwest while Mukpo was hospitalized — and whose blood type matched Mukpo’s. Mukpo left the hospital on October 22.
Back home in Providence, Mukpo opened up to the press about his experience. He thinks he got Ebola while interviewing patients outside a treatment center. But Mukpo, like Spencer, asks that we focus our attention on West Africa.
“The effects of the outbreak are going to be much larger than just the human toll of the medical crisis itself,” he says. He points out that the Sustainable Development Institute, shut down by the crisis, was one of the few groups scrutinizing the practices of foreign investors in Liberia. “There are still logging companies moving logs out of the country, mining companies moving resources out, plantation companies expanding into land that might be customarily owned by local communities,” he says. And, of course, small businesses have suffered, health services have evaporated, and basic social structures like the church and the family have been ravaged.
“It’s not just how many people die from Ebola,” Mukpo says. “It’s how the crisis reverberates throughout the whole country. I believe in the strength and resilience of Liberians, but it’s very unpredictable how this is all going to pan out in the next couple of years.”
Guinea
Anne Liu arrives in Guinea in mid-November to a welcome development: the United Nations Mission for Ebola Emergency Response (UNMEER) has collected thousands more mobile phones from donors. Liu has all the phones she needs: her long-range goal of building a comprehensive national information portal for Ebola response is becoming tangible. Liu and her team begin training the people who will train the contact tracers in the mobile-phone software. The November visit sees the first seventy-seven new contact tracers trained in Conakry, and some five hundred contacts entered into the database — people who have been exposed to Ebola patients, and whose health can now be tracked in real time.
Though news reports say that the spread of Ebola in Guinea has stabilized, November turns out to be a bad month: five hundred new cases, the highest monthly total yet in a country of twelve million — about the size of Ohio. By late December, a year from when little Emile Ouamouno got a fever in Gueckedou, the virus has killed more than 1,600 Guineans.
Still, Liu, back in Guinea for a third time in December, does not see a country turned upside down. In Conakry, kids play soccer in the streets. The markets are busy. People are “living as normally as they can,” Liu says. On the work side, there is a greater UN presence because of UNMEER; and interagency coordination, though not devoid of tensions, is stronger than it was in October. By late December, 130 contact tracers and twenty-seven supervisors have been trained and deployed; Liu anticipates another 650 contact tracers to be trained by January. The number of contacts being monitored has grown to nearly 1,300.
On December 24, WHO reports that more than three hundred new cases have been confirmed in the last three weeks, with “intense transmission” in Conakry.
To catch up with and beat Ebola will take valuable time. Liu’s wireless dragnet has been cast, and the race will go to the swift.
Sierra Leone
Across the border, the situation is far worse. By year’s end, the number of cases in Sierra Leone has climbed past nine thousand. Nearly three thousand people are dead (the true toll is thought to be much higher, due to unreported deaths). Hot zones have flared up in the western area of Freetown and in the eastern district of Kono, where eighty-seven bodies have been discovered, many of them piled up in a cordoned-off corridor of a hospital.
It is during this upsurge that ICAP sends a five-member team, led by Susan Strasser, back to Freetown. The British government has asked ICAP to evaluate the community care centers that have been going up. The original plan was to train laypersons to run the centers. But as the British military deployed these workers, it became clear that the severe conditions called for professionals. And so health workers from other African countries — Zimbabwe, Kenya, Ethiopia, Uganda — have been recruited to supplement the local workforce.
Out in the field, Strasser is encouraged by what she sees. The centers are up and running, and some have more beds than patients — “a good indicator that services are available and meeting the needs,” Strasser says. Still, in some places, “patients are dying in their homes, which is a separate issue of people not wanting to go to any health service.” At the units Strasser visits, she sees a caring treatment environment, where patients can be brought outside to see their family members. There is a growing perception, she says, that going to such a place is not necessarily a death sentence.
Strasser is heartened, too, by the sight of much more international activity than she’d seen in October. She tempers her optimism with caution: “The follow-on quality, support, supervision, and oversight of these units are things that need to be focused on,” she says. “You always have tension between quantity and quality.”
In a country with little more than a hundred doctors, outside help is vital. The foreign workers, says Strasser, “are doing an amazing job.” But they, too, will need help. On December 18, Sierra Leone took another hit: the country’s most senior doctor, Victor Willoughby, sixty-seven, succumbed to Ebola, five days after testing positive. He is the eleventh doctor to die.
By year's end, the programming on Star Radio is wall-to-wall Ebola: public-service announcements are shouted out. There are pop songs about Ebola, and discussions about the economic, political, social, and cultural effects of the epidemic.
Yinka Akinsulure-Smith wants to do more shows on Star Radio. People in Sierra Leone “are reeling,” she says. “To say the situation is upsetting is a total understatement. What’s particularly disturbing, in addition to all the deaths of the nurses and others, is that we’re losing doctors. That has been really, really upsetting. The feeling is, if doctors are dying, what hope do we have?”
A week before Christmas, Akinsulure-Smith stands in the offices of the African Services Committee on West 127th Street. About twenty people, some dressed in African clothing, sit before her. Minutes earlier, the audience heard committee attorney Kate Webster ’10LAW discuss the “temporary protected status” designation for Liberia, Guinea, and Sierra Leone that was made law by executive order on November 20. Now, Akinsulure-Smith prepares to lead a conversation on the Ebola-related problems faced by West Africans in New York: stigmatization, bullying, financial strain due to loss of business, and psychological hardship. But first, she has a small request.
“We have people back in our countries — in Sierra Leone, in Liberia, in Guinea — who are dying,” she says. “Who are infected. Who are ill. We have lost so many professionals — nurses, doctors. We’ve lost parents and children. And so what I believe is very important for us to do, to continue the conversation, is to observe a few seconds of silence in their memories.
“Please, rise, and let’s take a few seconds to remember those who are going on as a result of this horrible, horrible circumstance.”
There is a rustle of papers as everyone stands.
Silence. Seconds go by, and the speaker’s voice enters in a soft, clear tone, just above a whisper: “May their souls rest in perfect peace.”
An Unusual Virus
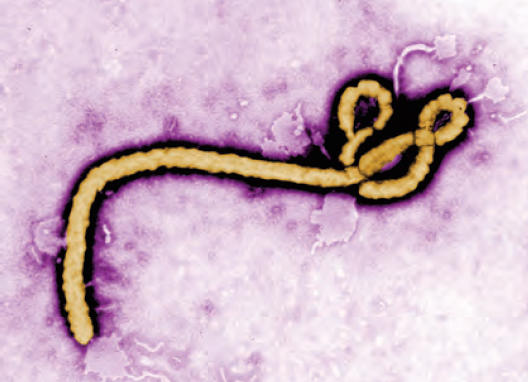
“One striking feature of Ebola is that, unlike most viruses, it replicates in a lot of tissues,” says Vincent Racaniello, a Columbia professor of microbiology and immunology who runs Virology Blog. “You can take the virus in through your mouth, nose, eyes, or skin, and it can spread throughout your body and grow in many different types of cells — in your respiratory tract, gut tract, skin, muscle, liver. That’s unusual for viruses. Usually, they’re restricted to just a few places, like influenza [respiratory tract] or polio [intestinal tract and nervous system]. We call that tropism: the cells and tissues where the virus replicates. Ebola is interesting because its tropism doesn’t seem to be regulated in any way.”
Like many scientists, Racaniello thinks that Ebola’s natural host is a fruit bat.
“All the viruses that we recognize in humans originated in animals,” says Racaniello, who in 1981 was part of the team at MIT that sequenced the poliovirus genome. “Influenza originates in birds, for example. Polio originated in animals, but now it’s strictly a human infection: it goes from person to person. But Ebola is not a human virus: every outbreak starts with the virus going from an animal to a human, and then it goes human-human-human, until we’re able to stop the transmission. The virus is then gone. When another outbreak happens, it’s from another animal entry,” probably from touching or eating an infected animal.
Once inside the human body, the virus works by entering a cell and then taking over the cell’s machinery to reproduce itself, making more Ebola proteins, which then break out of the cell and infect other cells.
“This is an RNA virus,” explains Columbia epidemiologist Stephen Morse. “Many viruses — Ebola, influenza, polio — have RNA genomes, and they all need their own special enzymes to copy themselves, because our body doesn’t know what to do with them. That’s why there are so many mutations in RNA viruses — those copying mechanisms are very sloppy. We don’t normally copy over RNA in our own bodies. DNA viruses like herpes simply use the DNA-copying machinery of our own cells.” Despite the profuse mutations caused by the RNA-copying process, neither Morse nor Racaniello see any real chance of the virus becoming airborne, as some people fear. “We have been studying viruses for over a hundred years,” Racaniello says, “and we’ve never seen a virus in humans change the way it is transmitted.”
As for the ghastly hemorrhaging — a result of damage to the cells that line the blood vessels — Morse says, “About 40 percent of cases get these dramatic Hollywood effects. So if you’re looking for that, very often you’ll miss the diagnosis.”