In a laboratory on the third floor of the Russ Berrie Medical Science Pavilion at Broadway and 168th Street, amid blue-capped test tubes and whirling centrifuges, glass beakers and humming refrigerators, there floats, in a petri dish, a pencil-eraser-sized piece of human scalp. Excised from behind the ear of a donor, the skin marinates in a clear solution like a baby scallop. Inside this bit of skin are hair follicles, and at the base of those follicles, in the hair bulb, reside stem cells, called dermal papilla (DP) cells. These cells, whose quantity in a hair follicle determines the dimensions of a hair — three thousand DP cells make a thick fiber, while three hundred make a baby-fuzz wisp — will be removed from the follicles and replicated, the first steps in a radical method to grow robust hair follicles in vitro, with the goal of transplanting them back into the donor’s head.
Humans are born with about a hundred thousand hair follicles in the scalp, with each one producing, over its lifetime, about twenty hairs. Our bodies don’t make more follicles: once they lose DP cells and shrink — a process called “miniaturization” — there is no way to restore them to normal size. But Angela Christiano, a professor of genetics and dermatology at the Vagelos College of Physicians and Surgeons, wants to plant new, DP-rich hair follicles in the ample spaces around the shrunken ones — which is just one facet of the boundary-shattering research flourishing in her lab.
Christiano made history more than twenty years ago when she became the first person to discover a gene for hair loss. Now, with her team of twenty technicians, grad students, and scientists, she is leading a multi-front attack on baldness, a condition that, in its various forms, affects eighty million American men and women. Hers is a tale of wild imagination and intellectual rigor: the daring geneticist who slashes through the unmapped jungles of hair-loss disorders, meeting dermatologists, immunologists, and biologists and forging collaborations that go beyond hair and into unforeseen territory, including cancer therapy.
Yet growing hair was the last thing on Christiano’s mind that spring day when her odyssey began, in the sweet aerosol haze of a beauty salon in Metuchen, New Jersey.
Bad hair day
“What happened?” said the hairdresser, ruffling her client’s dark, thick hair, which spilled lavishly from her scalp and tumbled past her shoulders. The stylist saw Angela Christiano every six weeks and knew the back of her head well. “Did you have a biopsy?”
A biopsy? Christiano didn’t understand. “No,” she said. “Why?”
“Oh,” said the hairdresser, “you have a small bald spot.”
It was May 1996. In the moment, Christiano didn’t think much of the remark. She was thirty, recently divorced, and six months into her job as a geneticist and professor at Columbia. During her postdoc at Thomas Jefferson University in Philadelphia, she had studied epidermolysis bullosa, a family of rare diseases that cause skin to become fragile and blister easily; now Christiano had her own lab in which to expand her research. With so much going on, she dismissed the small bald spot as an aberration, nothing to worry about.
But the next day at work, she asked a colleague to take a look. The colleague gasped. “It’s not small!” she said. The patch was the size of a coaster. Though Christiano studies the genetic foundations of skin diseases, she is not a medical doctor, so she made an appointment with a dermatologist. The doctor told her she had alopecia areata (AA), an autoimmune disease that runs in families. In AA, the immune system attacks the hair follicles, rendering them inactive and causing sporadic bald patches. Some people get alopecia totalis, which affects the whole scalp. The most extreme form, alopecia universalis, leaves the entire body hairless.
Christiano wasn’t shocked by the diagnosis: her mother and grandmother had suffered hair loss, and she had a second cousin with alopecia universalis. No, what really stunned Christiano was that doctors could not tell her anything more. They did not know what caused the disease, nor if her case would get better or worse or stay the same. The only treatment that modern medicine had to offer was steroid injections in the scalp, to calm the immune response — a painful prospect. Really? Christiano thought. That’s the best we’ve got? Her frustration, she remembers, grew into pure rail-at-the-gods rage. HOW DARE YOU MESS WITH MY HAIR? I’M FROM NEW JERSEY!
As a scientist, she figured there must be papers on the genetics of hair that would give her insight into what was happening to her, but there was virtually no literature to be found. How could that be? Christiano wasn’t sure. But she was looking for a new lab venture, and so, with nothing to lose, she applied for research grants to study AA. She quickly learned why there was so little progress on hair disorders.
“Institutions wrote back to me saying, in essence, that hair loss was trivial, cosmetic, insignificant in comparison to AIDS and cancer,” Christiano says today, seated in her office next to the lab. Her soft voice bubbles with humor and modesty. “Talk about frustration! The bar to getting funding for alopecia was so high, it was hard just to get in the door.”
Still, with doctors telling her that the only treatment for AA was shots in her scalp, Christiano felt she had no choice but to take her hair into her own hands. “As a geneticist, if I had any hope of untangling this disease, I had to lay the genetic groundwork.”
The hair-growth gene
Most of the estimated thirty-seven trillion cells in the human body contain, in their nuclei, our entire set of genes, about twenty thousand of them. Genes are the basic unit of heredity in all life forms, from people to plants to bacteria. Made up of discrete segments of DNA, a molecule shaped like a twisted ladder and coiled in threadlike bundles called chromosomes, genes encode messages for specific proteins to build and run an organism. They determine hair and eye color, send oxygen through the blood, and even control the expression of other genes. The entire chain of DNA in a cell is called the genome — the organism’s full set of chemical instructions.
The Human Genome Project — the sequencing of the three billion subunits, or base pairs, of the DNA molecule — gave geneticists a powerful new tool for identifying genetic factors in complex, multi-gene diseases. But in 1996, when Christiano ventured into hair genetics, the project was seven years from completion. At that time, no one had ever found a gene associated with the growth or loss of human hair. To get a genetic picture of hair loss, Christiano had to gain a foothold. She had to start small. That meant focusing on a simple, single-gene form of the disorder that might unlock understanding of forms involving more than one gene, like alopecia areata. She had to find a rare family with a parent-to-child-to-grandchild line of hereditary hair loss that was plainly the work of a lone rogue gene. “It really was like searching for a needle in a haystack,” she says.
Combing through a medical database, Christiano found two geneticists in Pakistan who were working with a family that had eleven members with a non-autoimmune form of alopecia that had left them totally hairless from infancy. Christiano knew that with such a genetically isolated type of baldness, the gene mutation would be noticeable. She asked the Pakistani scientists to send her blood samples.
Using automated sequencing, Christiano analyzed the family’s DNA and narrowed her search for the mystery gene to an area on chromosome eight. To pinpoint a hair-loss gene out of the nearly seven hundred genes on the chromosome was an imposing task. Fortunately, Christiano learned about a study in which hairless mice were born with fuzz that they quickly shed — which was what had happened in the Pakistani family. And since humans and mice have similar genetic structures, Christiano decided to compare the mouse gene with the family’s genes and look for a similar mutation. Incredibly, she found her needle: a gene that controls the growth of human hair.
A paper describing this discovery was published in Science in 1998. Given the widespread interest in hair loss, Christiano drew instant media attention. With her alopecia areata in remission after “many, many painful injections,” she appeared on TV and in magazines, explaining that the gene, called “the hairless gene,” or HR, was a kind of master switch for the hair cycle. This cycle has three phases — anagen (the growth of a hair, which lasts an average of three to five years); catagen (the cessation of growth, lasting two to three weeks); and telogen (a several-month dormancy, in which the hair follicle shrinks and the hair falls out). In the HR mutation, the switch that regulates this process is turned off, and hair cannot grow.
While this landmark finding did not herald an imminent cure for baldness, it did provide an enthralling glimmer, and Christiano got a substantial National Institutes of Health grant to create a DNA registry in the US for alopecia areata — the first step toward identifying the genes that cause that disease. That meant finding people from extended families in which multiple members had severe hair loss, as well as finding thousands of individual patients whose relatives were not affected. “All were valuable to the gene-hunting efforts,” Christiano says. The registry was compiled by Christiano at Columbia and four other institutions over a period of years.
For the AA community, this process felt endless. Still, year after year, at the annual conference of the National Alopecia Areata Foundation, for which Christiano is an adviser, attendees would, at her urging, roll up their sleeves and give blood, hoping that someday, somehow, the genes that caused their disorder would be found.
Attack of the killer T cells
In 2003, as Christiano and her colleagues continued to build the registry, the Human Genome Project was completed. This monumental international achievement allowed Christiano to conduct a much broader, more elaborate inquiry, called a genome-wide association study, in which samples from a thousand AA patients in the registry could be analyzed against the DNA of three thousand normal-haired counterparts.
Christiano secured an additional grant to perform the analysis. This haystack was far bigger than any she had ever searched, and she was amazed when the first pass turned up eight distinct genetic regions that were clearly different for sufferers and non-sufferers — “an incredibly good yield for only a thousand patients,” Christiano says. Since it took just eight regions of the genome, and not fifty or a hundred, to explain the genetic association underlying a thousand cases of AA, Christiano surmised that those regions must contain genes that play a predominant role in causing the disease. If a drug could hit some of those genes, it should work for the majority of patients.
Christiano then compared AA genes to the genes of other diseases, looking for similarities and differences. The results were a thunderbolt. “It turns out we don’t look like any other autoimmune skin diseases — not psoriasis, not eczema, not vitiligo,” Christiano says. “The autoimmune diseases we align with are type 1 diabetes, celiac disease, and rheumatoid arthritis. This was not at all what we expected.”
When she and her team looked at the literature on those diseases, they learned that all three use a similar signaling mechanism, in which wayward genes send out a “kill me” message that summons immune cells, or T cells, to target a healthy cell for destruction. Normally, when a damaged cell needs to be destroyed, the T-cell cavalry comes in, does its job, and stops. But in patients with AA, Christiano found, the signals that attract the killer cells to the hair follicles don’t turn off. “They’re always a little on,” she says.
But which gene was causing this to happen specifically in the hair follicle — and nowhere else? Which gene, in other words, was the “AA gene”?
“We geneticists want to find the genes that are unique to our disease,” explains Christiano. “There are plenty of other immune genes that are shared among diabetes and celiac and AA, but those just give you a generic susceptibility
to autoimmunity.”
The team zeroed in on chromosome six, where they detected what Christiano calls “the smoking gun for AA” — a gene called ULBP3. “This was the gene that landed us in the hair follicle,” Christiano says.
Nature published these findings on July 1, 2010. A few days before the journal came out, Christiano flew to Indianapolis to attend the twenty-fifth annual National Alopecia Areata Foundation global conference. Each year, Christiano would hear the stories of grief that so often accompany hair loss. She was especially moved by the plight of girls. “Girls who lose their hair as children and grow up that way are tougher — their identity has been formed without hair,” she says. “But girls who reach their teens with hair and then lose it — well, you can imagine. Boys, too. There’s a real difference between the kids who grow up with nothing and those who have it and lose it in the formative period. People who lose their hair at any time are certainly devastated, but those teen years can be particularly cruel.”
In the face of so much emotion, Christiano always rallied people at the meetings. She’d try to raise their spirits, while encouraging them to keep giving blood. “We’re getting there, we’re getting there,” she’d tell them. She could feel their frayed patience, the pressing weight of their hope.
But 2010 was different. It had been fifteen long years since Christiano discovered the first gene for hair loss. Now, at last, she had news to share about AA. She got up to speak, and the crowd of six hundred, many wearing scarves, caps, and bandannas, listened as she made her announcement: “I’m happy to say that this year, for the first time, we’ve finally found some genes.”
The room got quiet. Then people stood up. They began to weep, and, in a show of unity, they started taking off their head coverings. Christiano, unprepared for any of it, dissolved into tears.
Jersey roots
Growing up in Nutley, New Jersey, Christiano was surrounded by hair. Her mother, Maria, was a beautician in a hair salon. Her grandfather, Ernest Evangelista, an Italian immigrant, was a barber. As a kid, Christiano worked Saturdays at the salon, sweeping the snipped hair into fluffy multihued piles. She also served tea to the ladies there. Sometimes, women undergoing chemotherapy would come in and remove their wigs. Observing them, Christiano became sensitized to the powerful emotions around hair.
She was an only child. Her father, Angelo, was an Amtrak conductor on the Metroliner from New York to Washington and a proud member of the Masons. Neither he nor Maria knew precisely what to make of their daughter, who got hooked on science in eighth grade after reading an article about DNA in National Geographic. Christiano had an influential junior-high science teacher, a woman who was “very encouraging to girls,” she says. “She made science seem like an acceptable path.” At Nutley High, Christiano was one of two students selected for a work-study program at the nearby laboratories of the pharmaceutical company Hoffmann–La Roche. When she entered Rutgers to study biology, she became the first person in her family to go to college.
Later, as she began working on AA, Christiano learned more about the feelings that surround hair loss. “Because the condition is usually progressive, once it starts, people really struggle,” she says. “I’ve heard people say: ‘I couldn’t get out of bed.’ ‘I will not take off my hat.’ ‘I won’t go out in the wind because I’m afraid my prosthetic will come off.’ ‘I won’t be intimate with someone.’ ‘I can’t go on this job interview.’ ‘I’m afraid to show my family.’ Some patients have told me: ‘I can lose my hair, even my eyelashes. But when I lost my eyebrows I lost my identity.’ If they could just get back their own eyebrows, they could deal with almost anything.
“Then there is the unwanted attention from others, which is one of the most hurtful things. When you have an outwardly visible disease, the world feels that it’s all right to comment on it. ‘Are you having chemo?’ It’s like, Who the heck are you to ask?
“You need to walk a day in the shoes of someone before you cavalierly dismiss AA as ‘just cosmetic.’ It’s easy to trivialize it. But people are desperate, and vulnerable to the core. They’re up all night reading about hair and counting the hairs in the drain and looking in the mirror. You can’t understand it unless you’ve been there.”
Interdisciplinary tango
With her genome-wide study of AA done and her findings published, Christiano was at a scientific crossroads. The logical path was to move on and map other skin ailments. But she could not stop thinking about the resemblance between alopecia areata and non-dermatological diseases like type 1 diabetes, in which the immune system is tricked into attacking insulin-producing cells in the pancreas. The parallels enticed her; there was a thread she had to follow.
To do that, she would need help from outside her own field.
She did not have to travel far. CUIMC’s diabetes center is located below Christiano’s lab, and in 2010 Christiano went downstairs to greet her colleagues and get their opinion. They referred her to immunologist Raphael Clynes, then an associate professor of pathology and cell biology. Clynes agreed to meet with Christiano, who brought him stains of hair follicles that had been destroyed by T cells. Clynes looked at the images and said, “This is type 1 diabetes of the hair follicle.”
Now there were two people fascinated by the similarity. Christiano and Clynes began an intense collaboration. “As geneticists, not immunologists, my team didn’t know one end of a T cell from another, and he really took us under his wing,” Christiano says.
Clynes told Christiano about a new class of small-molecule drugs that disrupt the Janus kinase (JAK) pathway, one of the body’s main intercellular signaling systems. The drugs, called JAK inhibitors — there were two on the market — are used primarily for rheumatoid arthritis, in which the immune system attacks the joints. “Rheumatoid arthritis shares many signaling processes with AA,” Christiano says. Could the rheumatoid-arthritis drugs also block the killer T cells in alopecia areata?
Using mice with alopecia, the team found that the drugs, both as an oral and topical treatment, not only prevented alopecia but also revived inactive hair follicles. “The drugs did everything we had hoped they would do, and over time we became more and more skilled in understanding JAK pathways and defining the properties of an ideal JAK inhibitor to use for the disease.”
Christiano and Clynes published a paper in Nature Medicine in 2014 describing the mechanism by which JAK inhibitors prevented and reversed AA. The paper made waves. Columbia filed for related patents. Hoping to commercialize this intellectual property, Christiano and Clynes started a company called Vixen Pharmaceuticals. (“Vixen” is a play on the word “alopecia,” which derives from the ancient Greek alopex, meaning fox; alopecia in early medical literature is referred to as “fox mange.”) But the medicines still had to be tested on humans.
In 2016, Christiano got another grant, this one to further her quest for a painless treatment for AA. The grant required her to work with a medical clinician, and Christiano joined forces with Columbia dermatology professor Julian Mackay-Wiggan ’98PS, ’04PH, who had started testing JAK inhibitors on people soon after the mouse data had proved encouraging. Now Mackay-Wiggan and Christiano kicked the human trials into high gear.
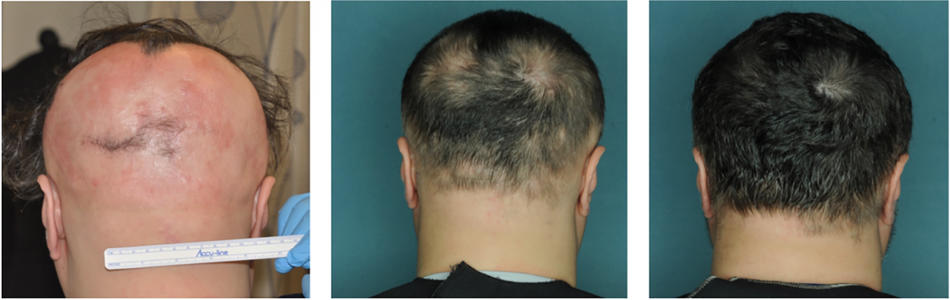
The results have been more than promising. Twelve AA patients were given the drug over a period of three to six months. Of the twelve, nine showed significant hair regrowth, and seven had regrowth of nearly 100 percent. The drugs are still in clinical trials and could gain FDA approval as soon as 2021. Since the Nature Medicine paper was published, at least six major drug companies have begun developing JAK inhibitors for alopecia areata. One of them, Aclaris Therapeutics, purchased Vixen Pharmaceuticals in 2016.
“For companies to take an interest in AA for its own sake, and not as a spinoff of psoriasis or eczema, is very gratifying,” Christiano says. “It’s a defining moment in the field.”
The cancer thread
When Mackay-Wiggan left Columbia for private practice, Christiano needed another medical researcher with an MD to satisfy a requirement of her grant. The answer was again just around the corner, this time at the Herbert Irving Comprehensive Cancer Center.
Columbia had recently recruited several immuno-oncologists — doctors seeking to harness the power of the immune system to fight cancer. One of them was Charles Drake, director of genitourinary oncology at CUIMC and a premier developer of new cancer immunotherapies. Christiano went to see him.
Though Drake was an immunologist working mainly on prostate cancer and Christiano was a hair-focused geneticist, the pair had an intriguing point of intersection. In treating alopecia areata, the goal was to prevent T cells from attacking the hair follicle. But in cancer, those same T cells were desirable, because they were the agents that killed the tumor. Christiano wondered: if oncologists are trying to attract those cells, could AA researchers learn from their work how to keep the cells out? And conversely: could oncologists use the master regulator of the AA immune response — the gene IKZF1, which is always turned on in AA — to draw
T cells to malignancies?
An algorithm developed by Christiano’s colleague James Chen ’13GSAS, a precision-medicine fellow at CUIMC, crunched data on thousands of cancer patients to find tumor types that had the IKZF1 gene in their cellular communication networks. The algorithm calculated that some cancers, including melanoma, would be receptive to AA T cells. Drake and Christiano went to work: they transplanted the faulty IKZF1 gene into mice with melanoma. Christiano knew that tumors in most cancer patients evaded the immune system. If she could trigger a tumor-
attacking immune response using AA genes, the implications would be huge.
Just as Christiano had hoped, the gene alerted the T cells, which invaded the melanoma and killed the tumor. The mouse study showed, further, that some types of cancer were able to turn off the IKZF1 gene, shielding the tumors from the immune system. But when the gene was turned back on, the cancers became vulnerable to the immune response.
Christiano and Drake published their findings in the July 25, 2018, issue of Cell Systems.
“Using our little autoimmune genes to potentially enhance melanoma immunotherapy is nothing we could have done alone,” Christiano says. “These collaborations create a whole other way of looking at the world.”
From one, many
There has never been a truly successful treatment for the most common form of hair loss, androgenetic alopecia, better known as male pattern baldness. Hair-transplant surgery merely moves functioning follicles from one site on the scalp to another, with no net gain of hairs, while drugs like Propecia and Rogaine only slow hair loss. And while Christiano’s lab has been able to revive dormant follicles in AA patients, the problem in male pattern baldness — the depletion of dermal papilla cells in the hair follicle — demands other strategies.
For more than twenty years, Christiano has been working with Colin Jahoda, a cell biologist at Durham University in England. Jahoda has spent his career doing microsurgeries in animals, moving follicle cells from one site to another. He implanted mouse whiskers into mouse ears and showed that a whisker could grow in another part of the body. In 1999, he took follicle cells from his own scalp and implanted them in his wife’s arm, which, four weeks later, sprouted scalp hairs: the first human-to-human hair transplant. Jahoda also discovered that cells from human hair follicles could engender new follicles in lab animals. But he lacked a genetics perspective, and that’s where Christiano came in.
“It was like music and lyrics,” she says. “Totally interdisciplinary. He’s a developmental biologist, we’re geneticists, and we were able to help put words to those phenomena for him, helping him learn the molecular language of what he had described over the years. And he taught us everything we know about surgery — how to micro-dissect the hair follicles and move the cells.”
Christiano had long believed that male pattern baldness was too common to have a strictly genetic basis: there must be many environmental and non-genetic physiological factors involved as well. Certainly, years of genetic studies had not led to any effective treatments. In order to attack the most prevalent types of baldness, Christiano would have to venture beyond DNA. She and Jahoda had an idea: since the body cannot produce new follicles, what if they could grow hair follicles outside the body, with the ultimate aim of implanting them in the scalp?
Experiments are underway, and the evidence has been tantalizing. In theory, that little scallop of scalp floating in the dish at the Christiano Lab could be the source of a full head of hair. Working toward that future, Christiano and her team harvest the cultured follicles and implant them in artificial skin built in the lab. This skin nourishes the follicle, prodding from it a colorless, keratin-protein filament. The team then removes the productive follicle and grafts it onto the skin of a mouse. The result? Hair growing out of mice — human hair.
Christiano expects to move these trials from mice to people in two to three years, bringing nearer the day when people can grow, in a lab, their own viable hair follicles — a limitless supply of one’s own hair.
“From one, many,” Christiano says. “That’s a beautiful technology.”
In 2016, Christiano and Jahoda started a hair-and-skin regeneration company specializing in stem-cell replication and re-implantation. They named it Rapunzel Bioscience, after the girl in the Brothers Grimm fairy tale. Held captive at the top of a tower, Rapunzel has only her long braids to connect her to the outside world. But Christiano’s own hair story gives the Grimms a run for their money: the beautician’s daughter who, after a brush with baldness, ascends the scientific tower, where she weaves a multidisciplinary ladder to hair regrowth and cancer therapy.
Yet it’s a true story. Christiano isn’t the type to make a big fuss about it, though. Even after she became a famous geneticist and a leader in hair research, her mother would joke that the fruit hadn’t fallen so far from the tree. “You do the same thing I do,” Maria Christiano would tell her daughter. “You just do it at Columbia.”
This article appears in the Spring 2019 print edition of Columbia Magazine with the title "The Rapunzel Effect."